Holt’s nutrition and health programs director, Emily DeLacey, shares about the current malnutrition crisis in Ethiopia, and how Holt staff and donors are helping to identify, feed and treat children.
While it’s never easy serving the most vulnerable and hard-to-reach populations, this is just the nature of going the distance to best serve children and families in need. And this is what Holt staff around the world and generous Holt donors do every day. In rural Ethiopia, this means faithfully serving thousands of single mother-headed households and children who have been orphaned.
But now, during this time of COVID, our challenges in Ethiopia have multiplied…
And our biggest concern for the children is malnutrition.
So many families were already struggling to eat, but now the pandemic has abruptly halted these families’ incomes and their ability to access food altogether.
COVID has impacted the entire world, including the most remote and rural areas of Ethiopia.
One of the greatest and most devastating effects for children is hunger and malnutrition. Here’s why:
- While on lockdown, families have been unable to work to purchase or grow food
- Children have stayed home and stopped attending health centers where they used to receive basic health care and nutrition screenings
- When schools closed, children at Holt-supported schools lost their free school lunch — often their best, or only, meal of the day
So many families were already struggling to eat, but now the pandemic has abruptly halted these families’ incomes and their ability to access food altogether.
The result? Malnutrition — and at a level that’s been devastating for children.
The Effects of Malnutrition
When children are abruptly cut off from consistent access to high quality food, this can result in acute malnutrition. Acute malnutrition differs from chronic malnutrition, where children and families may have limited access to high quality food, but still consistently have some. Acute malnutrition happens in response to abrupt changes in food systems or income — such as the result of conflict, a famine, or in this case, disruptions caused by the COVID-19 pandemic. This abrupt lack of food can result in children dramatically losing weight as their bodies begins to catabolize their small fat stores and their muscles.
Acute malnourishment causes something called “wasting” — appropriately named as it appears that a child’s body begins wasting away. They get bone-thin arms and legs, distended bellies, visible ribs, sunken eyes and more. At a certain point, children don’t even act hungry anymore. It’s heartbreaking to see.
When a child is malnourished, they’re also more likely to become sick with illnesses, including COVID, and are less likely to recover. Many of these children additionally suffer from chronic intestinal parasites or diarrhea — common in rural communities like those we serve in Ethiopia. These illnesses prevent the nutrition they consume from being utilized by their bodies to help them grow. Instead it is used by the parasites to multiply. These conditions, when combined and left untreated, can be deadly.
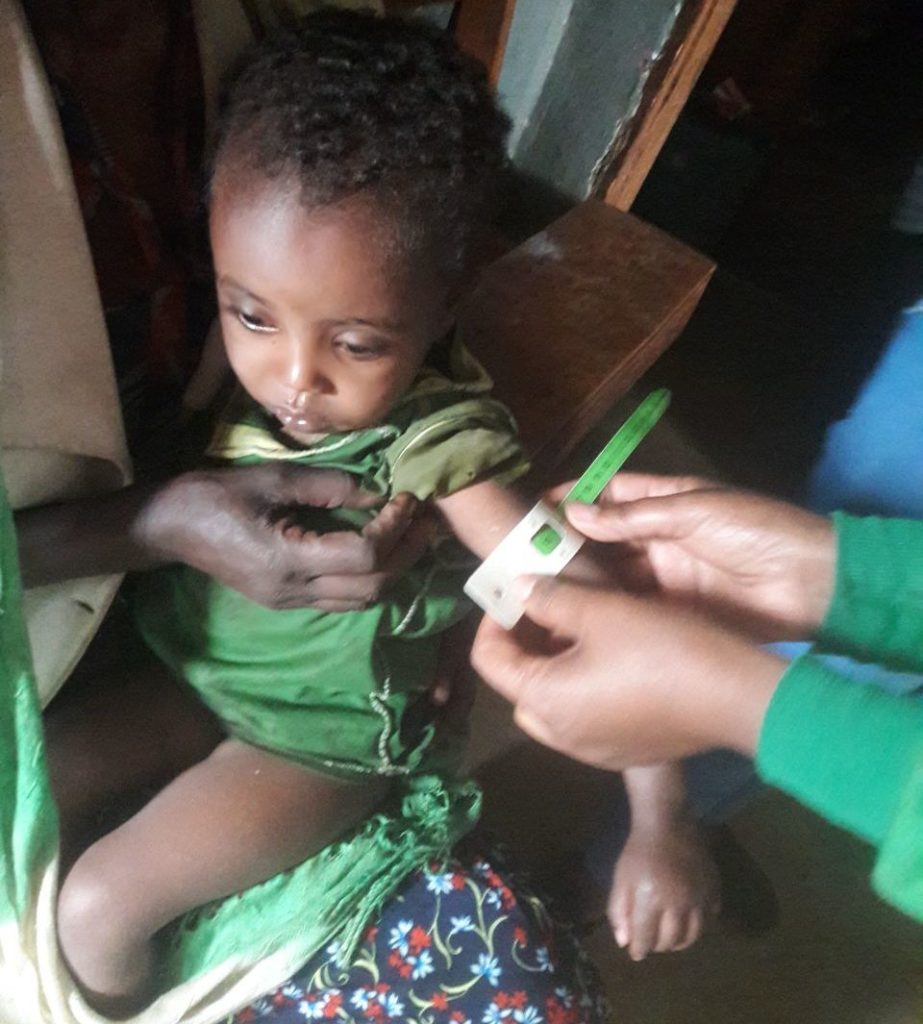
Holt’s Response to Malnutrition
The fear of children experiencing acute malnutrition has led our Holt Ethiopia team and our government partners to mobilize an emergency response. They started by screening as many children under 5 as possible for malnutrition. With support from Holt staff, skilled community health workers went door to door in full protective gear to safely assess children.
Incredibly, they reached more than 13,000 children under the age of 5. While in families’ homes, the health workers also shared vital COVID-19 information — helping families understand how to stay safe and healthy.
Feeding and Treating Children
However, malnutrition screenings were just the first step. Of the over 13,300 children screened, 5,797 were acutely malnourished. It was already starting to show in changes in their bodies and faces. These children needed urgent attention.
For the most in-need children and families, our health care workers distributed emergency nutrition packets in the field. But treating malnutrition is neither quick nor simple. Over the next months, the families of malnourished children received individualized nutrition training, and help for increasing their income and accessibility to food. These children will continue to be regularly screened and monitored until their malnutrition is fully treated.

The most dangerously malnourished children were transferred to Holt’s Mother and Child Hospital, where they received intensive nutrition intervention — therapeutic nutrition formula given under the exert care of medical professionals.
Thanks to our donors, children are receiving the critical nutrition intervention they need. But the more our Holt Ethiopia team goes out in the field, the more and more malnourished children they find. That’s why this program is so important, and the support of Holt donors is so needed and critical.
Together, we aim to serve every child who is hungry and malnourished. Because every child deserves to be healthy and grow to their fullest potential.
Emily DeLacey MS, RDN, LDN is a registered and licensed dietitian/nutritionist and a PhD candidate with the London School of Hygiene and Tropical Medicine. As director of Holt’s nutrition and health programs, Emily has managed nutrition intervention and behavior change programming in more than 15 countries. She is passionate about advocating for the nutritional needs of children and families.







Emily, amazing work, thank you!