Earlier this year, Holt organized a medical campaign to the Shinshicho/Durame region of Ethiopia. Six American physicians — several of them Holt adoptive parents — volunteered a week of their time and resources to treat patients in this rural, impoverished area of the country. Over the week, they saved several lives. Some in truly extraordinary ways.
Earlier this year, six American doctors traveled to southern Ethiopia as part of a medical team trip organized by Holt. They visited two healthcare facilities – a small health clinic in Shinshicho, and a hospital in neighboring Durame. Here, they were joined by two Ethiopian doctors who traveled from the city to help treat patients in this rural, impoverished region of the country.
Over the week-long campaign, they saw conditions rarely seen in the U.S. Goiters caused by iodine deficiency. A 3-year-old with legs paralyzed by polio. Malaria. Advanced wounds. And patient after patient with prolapsed uteruses and bladders – a consequence of constant physical labor, poor nutrition and long hard childbirths, often at a very young age.
They also met children that tugged at their hearts with soulful eyes and failing hearts or lungs. Some they had to turn away, unable to help them. Their conditions were too serious, the hospital’s resources too few.
But several lives, they did save. In one little one’s case, all it took was a little ingenuity, and an empty plastic water bottle.
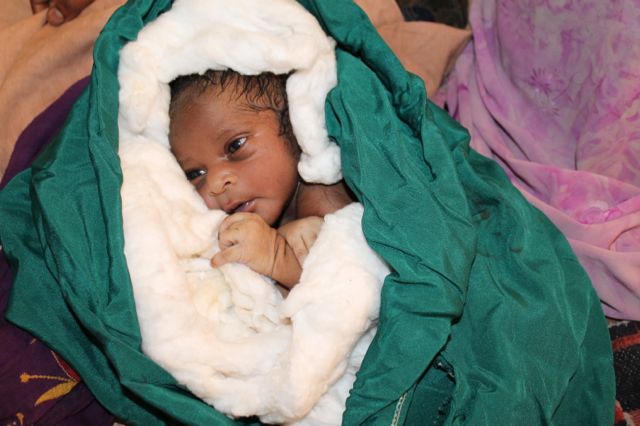
Dr. Kristen Bannister is an OBGYN

“One of them looked just horrible,” she says. “Because he was working so hard to breathe, his ribs were flaring out and his stomach was sucked in. He was burning hot with fever.” The boy’s aunt sat with the 3-year-old boy, looking helpless as her nephew struggled to breathe.
Catching the local medical staff on daily rounds, Dr. Bannister called their attention to the sick baby. “The doctor said the baby was having an asthma flare, but they didn’t have the meds to treat it,” she says. With few options, they did what they could – giving him Tylenol to treat his fever, and starting him on antibiotics.
What happened next, they would have to just wait and see.
The “wait and see” approach is not uncommon in this region of Ethiopia – a rural area so limited in access to medical care that one in ten children die before the age of 5, most from preventable or treatable illnesses. Here, a child might die from an asthma attack while in hospital care, simply because they lack the medicine to treat him. When a child enters care with a more complex health condition, praying for recovery often seems the only option.
This was the case with one young boy the doctors met in Durame.
Born with a congenital heart defect called tetralogy of fallot, the boy would need a series of four or five surgeries to repair his heart. At the hospital, the boy’s father kept coming up to the medical team throughout the day – “begging us with his eyes to help him,” says Dr. Bannister. “Both the boy and his dad had very soulful eyes.” But none of the visiting or resident medical staff had the specialized skills to fix his heart. “They would need a pediatric cardiac surgeon who specializes,” she says. “You’re not going to get that in that area.” In fact, nowhere in Ethiopia – not even in Addis Ababa, Ethiopia’s capitol city – is there a doctor trained to perform pediatric cardiology surgery.
“He took all of our hearts,” she says.
For this boy, the outlook was not a hopeful one. His heart was failing fast. But for the 3-year-old struggling to breathe from half an oxygen cannula, there was still hope. And with any small glimmer of a chance the boy could survive, the medical team would do more than just wait and see.

As the oxygen cannula seemed not to be working, Dr. Bannister got creative – rigging a surgical mask to help him breathe easier.
“His pulse ox was reading 65. Normal would be 95-100 for a healthy baby,” she says, referring to the amount of oxygen in his blood. With the mask, his reading went up to the low 90s. But without the proper equipment to keep the mask in place, his aunt had to hold it up to the boy’s face to ensure a steady flow of oxygen. The baby kept fighting it, and Dr. Bannister doubted he would keep it on for long.
“After lunch, I asked if Laurie and Becca would go see the baby,” says Dr. Bannister, referring to Laurie Clarkston and Becca Brandt, two of the six American doctors who traveled as part of the Holt medical team. A Holt board member, Dr. Brandt has led several previous medical campaigns to this region of Ethiopia. Dr. Clarkston is a Holt adoptive mom to three children from China. She first admitted the boy to the pediatric ward after noticing his condition the previous day.

Upon entering the ward, they saw that the baby had taken off the mask. “He was barely moving, still getting barely any oxygen,” says Dr. Bannister. Dr. Brandt immediately got one of the house officers – the local medical staff – and together they went down to the pharmacy to get an inhaler.
“The pharmacy only had one inhaler on the entire list – one you’re not supposed to use in kids or in acute situations,” says Dr. Bannister. The inhaler also cost about two dollars, an amount exceeding the means of many families in this impoverished area. As it was the only available medicine, Dr. Brandt bought it anyway – using her own money because the family couldn’t afford it.
“The medicine we gave him was not something I would ever give a child who had what he had,” says Dr. Clarkston, a family practitioner from Missouri. “But we had no other choice.”
When Dr. Brandt returned to the ward, the doctors attempted to administer the medicine. “It was an inhaler,” says Dr. Bannister. “As you push it down, the person has to breathe it in at the same time, which is hard to do in babies – especially when they’re not feeling well.” When they pushed down, the inhaler sprayed everywhere. It wasn’t working. The baby was not inhaling any of the medicine.
At this point, several of the medical team doctors had gathered around the patient, including Dr. Herb Whinna – a pathologist from Hillsborough, NC and father to two girls adopted from Ethiopia. Dr. Whinna suggested using a spacer, a device that sprays the medicine at a slower, more controlled rate. But as they would be hard pressed to find a spacer in rural Ethiopia, Dr. Whinna headed for the cafeteria.

“He had seen one done with a plastic bottle on a previous medical missions trip,” says Dr. Bannister. After grabbing an empty bottle from the cafeteria, Dr. Whinna taught the local nurses how to spray the meds to deliver the medicine to the baby. It worked! The baby could finally breathe, and all of the doctors sighed with relief.
“The next day, the baby was looking perky and great,” says Dr. Bannister. “All he needed was a day of antibiotics and the spacer. Without that, it would not have worked.”
Had the medical team not treated the baby, Dr. Bannister says it’s hard to say what would have happened. “There was a chance the boy would not have survived,” she says. “If he had lived, with that little oxygen, he could have had brain damage.”
In this baby’s case, the team was able to improvise a solution using the resources available at the hospital in Durame. The boy survived, and all is well. But given access to modern medicine and equipment, a simple respiratory virus should never escalate to a life-or-death situation. “In the U.S., he would have come in and had nebulizer treatments, antibiotics and that would have been it,” says Dr. Bannister. “Even in the most basic clinics here, they have those resources.”
Not so in rural Ethiopia. “Medically, there are so many needs there,” says Dr. Clarkston. At both facilities, the medical team worked without running water – scrubbing for the OR with tap water from a bucket full of leaves and debris. They used scalpels that had no handles – just a thin blade between their fingers to make delicate surgical incisions.
“The facilities themselves, I was surprised – they were bigger than I had anticipated and had better staffing than I anticipated,” Dr. Bannister says of

the Durame Hospital. “But they really didn’t have any materials to work with. The lab, X-ray machine and ultrasound were all very basic.” The hospital had one oxygen monitor, which sometimes worked and sometimes didn’t. The thyroid machine was broken the week they visited. The kidney machine, also broken.
“There was a lot of dealing without, monitoring-wise,” says Dr. Kendle Yates, an anesthesiologist from Tennessee. “There was maybe one set of functional equipment shared between two rooms. They picked the patient who was sickest to receive the monitoring.” Dr. Yates has traveled overseas on several previous medical mission trips with other organizations. By comparison with other developing countries he has visited, the state of care in rural Ethiopia was disheartening. “They don’t have the infrastructure or medicines that they have even in Guatemala where I’m used to providing care,” he says.
In the case of babies born prematurely, inadequate or nonexistent equipment significantly affects their chance of survival. “They don’t have an incubator,” says Dr. Clarkston. “So when they have a preemie, they use Kangaroo care, which means skin-to-skin contact with Mom. But if that isn’t enough, they have no way to keep the baby warm.”
And without running water, sanitation becomes a major issue. “One day, we had so many surgeries that we had to cancel the rest because they didn’t have enough clean equipment ready to go,” says Dr. Hanlon, an OBGYN from New Hampshire.
Here, at the Durame Hospital, is where the medical team spent most of the week. Between the Durame Hospital and Shinshicho health clinic 45 minutes away, Durame, says Dr. Hanlon, was the more functional of the two.

Four years ago, Holt came alongside the people of Shinshicho to help improve healthcare services in their community. With limited resources and staffing, the local clinic served few patients. Most people opted to travel the 12 miles to the hospital in Durame – often on foot. After Holt completed renovations to the clinic and hired a full-time medical doctor, the number of people receiving care more than tripled. The Shinshicho medical staff treated people for malnutrition and diarrheal diseases, malaria, HIV and leprosy, and respiratory infections such as TB. To encourage more women to deliver their babies at the clinic rather than at home, Holt also refurbished the delivery rooms. But the clinic was still just a clinic. For anything beyond basic outpatient care, Shinshicho residents would still have to travel to Durame.

While in Durame, the medical team doctors saw several patients who had traveled from Shinshicho for treatment. “It was quite impressive how far people would walk for health care,” says Dr. Bannister. “Some might walk 10-15 miles with a sick one to get to a lab or stay the night.”
“Some are sick and on foot,” says Dr. Hanlon. “But that’s how far away the nearest decent hospital is.”
In 2010, Holt and the Shinshicho community came together to remedy this problem – with Holt committing to fund most of the construction costs for a full maternal-child hospital. With support from the community in both funding and labor, Holt completed the internal structure of the hospital at the end of 2012 – leaving just one final construction phase. Once complete, the Shinshicho Mother & Child Health Center will provide acute, quality care for a region of 250,000 people. It will be equipped with surgical theaters, labor and delivery rooms, emergency and intensive care units, as well as the hot running water needed to wash and sanitize equipment and linens.
“It will be a huge improvement in their access to care,” says Dr. Clarkston.
At Holt’s headquarters in Eugene, Oregon, two giant containers full of medical equipment sit awaiting shipment. Donated by local hospitals and collected by a Holt supporter and adoptive parent, the equipment includes everything from sheets, blankets and gowns to exam tables, wheelchairs and an ultrasound machine. For additional supplies and medicines needed to fully equip the hospital, Holt is working with the government of Ethiopia.
“Holt will have a long-term, ongoing relationship with the Mother & Child Health Center,” says Dan Lauer, Holt VP of programs in Africa and Haiti. Among other efforts, Holt will help facilitate training opportunities for the local medical staff.
“I definitely think there are opportunities for people to come in – definitely in pediatric and neonatal and do some teaching with them,” observes Dr. Bannister. “The people are so receptive to help and so gracious and I think there is the potential for a great working relationship with them.”
Although they had limited equipment, supplies and training in some areas, the overall resourcefulness and skill of the local Ethiopian staff impressed the visiting medical team. “You can’t imagine working in that setting, but it’s amazing how well they do with what resources they have,” says Dr. Clarkston.
When Dr. Yates arrived in Durame, he discovered that two other local anesthesiologists had traveled from Addis to provide services. As the third anesthesiologist on site, he was not able to contribute his services as much as the other doctors. But he took the opportunity to observe how the local physicians worked with fewer resources and medicines. “I learned by seeing what they typically did with what little resources they have,” he says.
“Both the visiting surgeons and the resident doctors were very skilled,” agrees Dr. Hanlon. “They are well-trained, excellent surgeons and showed tremendous dedication.”

For all the participating doctors, the medical team trip provided a unique opportunity to see Holt’s work in Ethiopia firsthand. They treated patients in a clinic Holt refurbished and staffed, and at the Durame hospital – where Holt has been instrumental in bringing in needed physicians. They saw the Shinshicho Mother & Child Health Center, nearly complete. They also met children in Holt sponsorship, and families in our family strengthening and preservation programs.
“I had no idea what Holt did in country, and to see the difference Holt is making in these families’ lives is very impressive,” says Dr. Clarkston. As an adoptive parent, Dr. Clarkston felt a personal connection to Holt’s work in country. “It makes you feel better knowing that your kids were well taken care of,” she says.

For Dr. Hanlon, the trip was especially meaningful.
In 2008, Dr. Hanlon traveled to Addis, Ethiopia with her husband to bring their daughter Medhanit – “Meddy” – home. Five years later, the medical team trip for the first time took her to the region where her daughter was born. Here, she had the opportunity to meet her daughter’s grandparents – Meddy’s only living relatives. “It was very special and emotional,” she says. “For them to see pictures of her, and see

how beautiful and happy and healthy she is, they were overjoyed.” Dr. Hanlon was able to communicate with Meddy’s grandparents through a translator, and take pictures and video for her daughter. “To meet her family and bring everything full circle, that was really important – for me and for Meddy,” she says. One day, Dr. Hanlon hopes to bring Meddy back to Ethiopia. “It’s part of who she is and what makes her special,” she says.
The chance to observe Holt’s work in her daughter’s birth country also helped bring everything full circle for Dr. Hanlon. “Seeing the families and the hospital and how much Holt is doing for Ethiopia and how many lives have been impacted in the country… I’m so impressed,” she says.
For Dr. Yates – a Holt adoptive parent and adoptee from Korea – the trip’s meaning transcended connection to country and culture, and even connection to Holt. “It really doesn’t matter where we go,” he says, “as long as we’re out to help people and share love with others.”
During the week, the doctors had many joyous successes – saving and improving the lives of children and families. Other patients, they could not treat. These losses were made more heartbreaking because somewhere else – somewhere with the proper equipment and medicines and specialists – they could have helped them. But as Holt continues to work alongside the community to strengthen healthcare services, fewer and fewer lives will be lost unnecessarily. Once complete, the Shinshico Mother & Child Health Center will have the capacity and resources to treat thousands of patients who might never otherwise receive treatment.
As Dr. Bannister says, “It will have a phenomenal impact.”
Robin Munro | Senior Writer

Learn more about Holt’s work in Ethiopia!
See how sponsors and donors create a brighter, more hopeful future for children and families in Ethiopia!





